Move Against Cancer Africa | January 2026
In a busy oncology ward in Lagos, a 38-year-old mother of three lay quietly, her strength drained after multiple cycles of chemotherapy. Her doctors were ready to continue treatment- but her blood counts had crashed. Without an urgent transfusion, the next phase of care could not proceed.
Her blood group was O negative, one of the rarest and most demanded types. Family members were tested. None matched. Calls went out to blood banks across the city, then across the state. With no immediate donor among family and friends, clinicians reached out to multiple blood banks. One by one they checked stocks. Nine had nothing suitable. On the tenth call, a matching, screened unit was finally available. That single bag of blood didn’t just stabilize her- it kept her cancer journey alive. Across Nigeria and Africa, this scenario plays out far more often than we realize.
A Critical Gap in Cancer Care
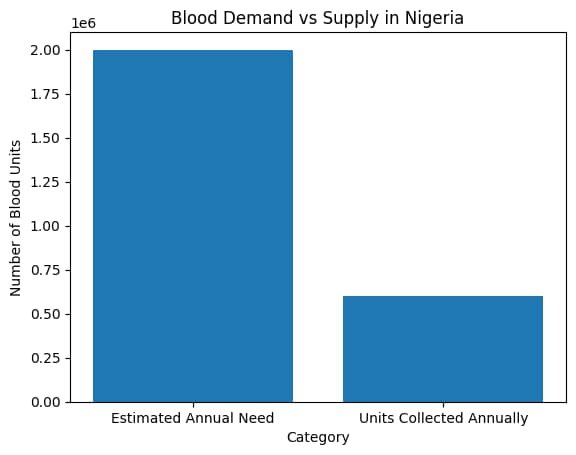
Cancer care does not end with chemotherapy, radiotherapy, or surgery. For many patients, blood transfusion is a lifesaving necessity, especially for those experiencing treatment-induced anemia, bleeding, or bone-marrow suppression. Yet Nigeria faces a severe blood supply crisis. According to the World Health Organization (WHO), countries need blood donations equivalent to 1% of their population annually to meet basic health needs (WHO, 2023). For Nigeria’s population of over 200 million, this translates to nearly 2 million units per year.
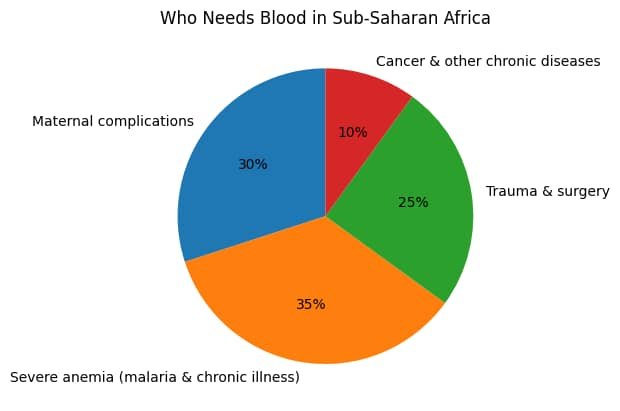
However, national estimates show that less than 30% of this need is currently met, with voluntary, unpaid donors contributing only a fraction of collected blood (WHO AFRO; National Blood Transfusion Service, Nigeria). Across sub-Saharan Africa, the challenge is even broader. Blood shortages affect care for maternal hemorrhage, trauma, severe malaria, and increasingly, non-communicable diseases such as cancer (WHO AFRO, Blood Safety Programme).
When blood is unavailable, cancer treatment is delayed, doses are reduced, or care is abandoned entirely.
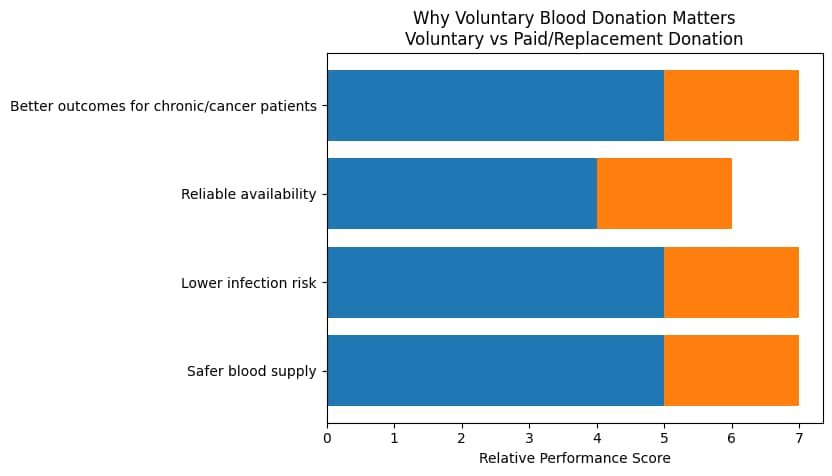
What the Evidence Shows
The data behind this crisis is consistent and alarming:
Africa accounts for about 25% of the global disease burden but collects only ~5% of the world’s blood supply (WHO AFRO, 2022). In Nigeria, most blood donations still come from family replacement or paid donors, rather than voluntary non-remunerated donors recommended by WHO for safety and sustainability (WHO, 2023).Patients with high-demand blood types, particularly group O and Rh-negative types, are most affected during shortages. Cancer patients often require multiple transfusions over the course of treatment, increasing their vulnerability in low-supply settings (WHO Cancer Control Programmes).
The implication is clear: blood availability directly influences cancer survival outcomes.
The Lagos patient survived because blood was available at the last moment. But for many others across Abuja, Enugu, Kano, and rural communities, that tenth blood bank never comes through. Doctors see these daily: Cancer patients waiting days for transfusion, families desperately searching for donors, treatment schedules disrupted due to low haemoglobin levels.
Behind every successful transfusion is a fragile chain:
the donor → the blood bank → the laboratory → the health worker → the patient.
When one link fails, lives are lost quietly and preventably.
Why blood donation must be central to cancer advocacy
Blood donation is not optional support; it is core cancer care.
Without safe, timely blood transfusion, modern cancer treatment simply cannot function. Strengthening blood systems is as important as expanding oncology centres or introducing new therapies.
Cancer advocacy must therefore include:
1. Voluntary blood donation.
2. Safe and ethical blood banking.
3. Policy investment in national blood systems
A call to action: Your blood can save a cancer patient
At Move Against Cancer Africa, we believe no cancer patient should lose their chance at survival because blood was unavailable.
This month, we call on:
🔴 Individuals: Become a regular, voluntary blood donor, especially if you have group O or Rh-negative blood.
🔴 Institutions & Employers: Host blood drives and normalize donation as civic responsibility.
🔴 Communities & Faith Groups: Promote blood donation beyond emergency appeals.
🔴 Policymakers & Partners: Invest in sustainable, voluntary national blood systems.
For someone fighting cancer, your blood could be the difference between delay and cure, despair and hope, life and loss.
Let us act, before the shelves run dry.
To find out how you can donate blood, check the National Blood Transfusion Service website in your region and visit the nearest blood transfusion centre.
Move Against Cancer Africa: Advancing equitable cancer care across Africa – one life, one donation, one system at a time. 🌍🩸
Authors: Dr Abiodun Egwuenu, Mrs Ogechukwu Akabuike
References
1. World Health Organization (WHO). Blood Safety and Availability. WHO AFRO.
2. WHO (2023). Global Status Report on Blood Safety and Availability.
3. Nigeria National Blood Transfusion Service (NBTS).
4. WHO Cancer Control Programmes: Supportive Care.





